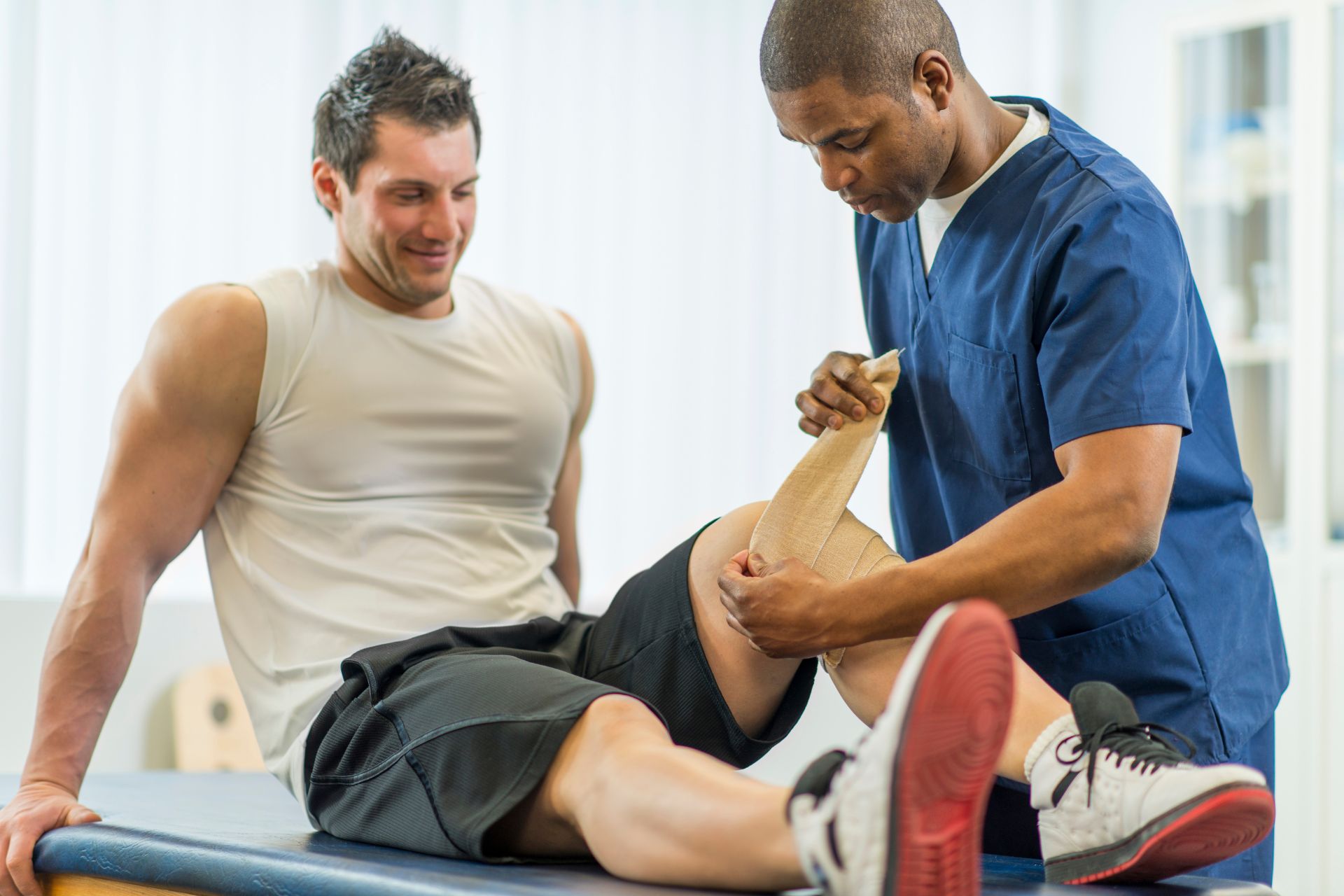
Frequently Asked Questions
Post-operative knee rehabilitation for orthopedic patients typically involves a carefully structured regimen of exercises aimed at restoring strength, flexibility, and functional mobility. Initially, gentle range-of-motion exercises, such as heel slides and ankle pumps, are crucial for reducing stiffness and promoting circulation. As healing progresses, patients may incorporate isometric quadriceps contractions and straight leg raises to enhance muscle activation without placing undue stress on the joint. Strengthening exercises, including wall sits and step-ups, are essential for rebuilding muscle strength around the knee, while balance training, such as single-leg stands, helps improve proprioception and stability. Additionally, low-impact aerobic activities, like stationary cycling and swimming, can be beneficial for cardiovascular fitness without exacerbating joint pain. Throughout the rehabilitation process, it is vital to monitor pain levels and swelling, ensuring that the exercises are tailored to the individual’s recovery stage, ultimately facilitating a safe return to daily activities and sports.
When modifying physical therapy exercises for patients with chronic lower back pain, it is essential to consider individual pain thresholds, functional limitations, and specific diagnoses such as lumbar disc herniation or degenerative disc disease. Incorporating low-impact activities like aquatic therapy or stationary cycling can alleviate stress on the lumbar spine while promoting mobility and flexibility. Strengthening exercises should focus on the core stabilizers, including the transverse abdominis and multifidus, using techniques such as pelvic tilts and modified planks to enhance spinal stability without exacerbating discomfort. Additionally, integrating gentle stretching routines, like the cat-cow stretch or child’s pose, can improve lumbar flexibility and reduce muscle tension. Utilizing modalities such as heat therapy or electrical stimulation may also complement the exercise regimen, facilitating pain relief and enhancing overall functional capacity. Regular assessments and adjustments to the exercise program are crucial to ensure safety and effectiveness, allowing for gradual progression based on the patient's response and tolerance levels.
After hip surgery, incorporating specific stretching techniques is crucial for enhancing hip mobility and promoting recovery. Gentle static stretches, such as the seated butterfly stretch, can effectively target the adductor muscles, while the figure-four stretch helps to improve external rotation and flexibility in the hip joint. Dynamic stretches, including leg swings and hip circles, facilitate blood flow and increase range of motion, essential for rehabilitation. Additionally, the use of foam rollers for myofascial release can alleviate tension in the surrounding musculature, further supporting mobility. Incorporating hip flexor stretches, such as the lunge stretch, can also counteract tightness and improve overall hip extension. It is important to perform these stretches within a pain-free range and gradually increase intensity, ensuring that the recovery process is both safe and effective.
Effective strengthening exercises for shoulder rehabilitation following a rotator cuff injury focus on enhancing the stability and functionality of the shoulder joint while promoting muscle balance. Key exercises include external rotation with resistance bands, which targets the infraspinatus and teres minor muscles, and internal rotation exercises that engage the subscapularis. Scapular stabilization exercises, such as wall slides and scapular retraction, are crucial for improving the overall mechanics of the shoulder girdle. Additionally, incorporating isometric shoulder abduction and flexion exercises can help in gradually rebuilding strength without excessive strain. Progressive resistance training, including the use of dumbbells for lateral raises and front raises, can further enhance deltoid and rotator cuff muscle strength. It is essential to emphasize proper form and controlled movements to prevent re-injury and ensure effective recovery. Overall, a comprehensive rehabilitation program that includes these specific exercises can significantly aid in restoring shoulder function and strength post-injury.
Aquatic therapy can be effectively integrated into an orthopedic rehabilitation program for patients recovering from joint replacements by utilizing the unique properties of water to enhance mobility, strength, and overall functional recovery. The buoyancy of water reduces the impact on weight-bearing joints, allowing patients to perform therapeutic exercises with decreased pain and increased range of motion. Hydrostatic pressure aids in reducing edema and promoting circulation, which is crucial for healing post-surgery. Specific aquatic exercises, such as resistance training with water weights or aquatic walking, can be tailored to target the muscles surrounding the replaced joint, thereby improving stability and proprioception. Additionally, the warm water environment can facilitate relaxation and decrease muscle tension, further enhancing the rehabilitation process. By incorporating aquatic therapy into the rehabilitation protocol, clinicians can provide a comprehensive approach that addresses both the physical and psychological aspects of recovery, ultimately leading to improved outcomes and a quicker return to daily activities for patients with joint replacements.